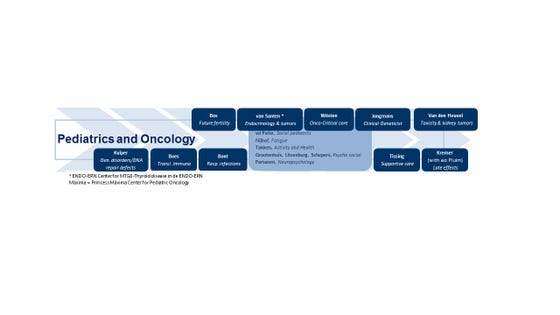
Pediatrics and oncology
Pediatrics and oncology
Around 600 children in the Netherlands are diagnosed with cancer every year. Thanks to medical advancements, an increasing number children with cancer survives and grows up into adulthood. Childhood cancer survivors are at increased risk of psychosocial and physical health problems. The pediatric care for these children is embedded through the collaboration with the Princess Máxima Center. This enables a unique cohort composition with expertise regarding pediatric tumors as well as physical and psychosocial early and late adverse effects of cancer treatment.
Participation in scientific research uitklapper, klik om te openen
Marit, daughter of the Kirstmann family, was diagnosed with leukemia (blood cancer) when she was just one year old. At the age of two she underwent a stem cell transplant as well as extensive chemotherapy treatment. She was subsequently monitored for possible late effects of that treatment and continues to come in regularly to the Late effects outpatient clinic where she has attended from the age of six.
"Marit is now seen once a year at the Late effects outpatient clinic where her doctor examines her to see how she is doing. Marit's illness takes a back seat, the focus now being on her future."
Participation in scientific research
Lifecycle uitklapper, klik om te openen
Since 2018, all children with cancer in the Netherlands are being treated in the Princess Máxima Center in Utrecht. Care is provided for the very young infants throughout adolescence. Both the Wilhelmina Children’s Hospital (WKZ, with the chair working in Prospective Pediatrics (van de Putte)) as well as the Princess Máxima Center have a focus on the consequences on health related quality of life. It is considered important to minimize the influence of disease during childhood on physical, emotional, cognitive and social functioning.
The investigators within Child Health aim to improve lifecycle care, which is made possible by the excellent collaboration between the Wilhelmina Children’s Hospital, the UMC Utrecht and the Princess Maxima Center. Transition of care is one of the main themes of paediatric care during and after cancer treatment, as well as for care as for research.
Interdisciplinairy uitklapper, klik om te openen
Pediatric research in children with or surviving cancer is always interdisciplinary. All researchers of the post-oncology theme within Child Health collaborate with different researchers from all fields of medicine within the Princess Maxima Center; of which most important are the late effects Group (prof. dr. L. Kremer), the supportive care group (W. Tissing) , and the departments neuro-oncology (E. Hoving), solid tumors (J. Zsiros, S. Terwisscha), hemato-oncology (J. Vormoor, F. Wentrup-Meyer) and stem cell transplantation (M. Bierings). Also strong collaboration exists with the departments of physical therapy (T. Takken, P. vd Torre). Important collaborations also exists with departments within the UMCU, such as the fertility department (A. Bos), endocrine oncology (G. Valk, M. Vriens), clinical genetics (M. Jongmans), pathology (P. Wesseling, R. de Krijger). National collaboration is present with different academic hospitals. Important international collaborations have been formed with the St. Jude Children’s Research Hospital, with the International Group Harmonization Guidelines (IGHG) and the POKER collaboration (Pediatric Oncology Kids in Europe Research group, UK, Germany, Belgium, France, Denmark, the Netherlands, Switzerland).
Physical & mental development uitklapper, klik om te openen
Childhood cancer is a highly multi-faceted multi-organ disease. Physical exercise and well-being is an important aspect of pediatric care during cancer treatment and is embedded by the research line of T. Takken with the medical physiology department WKZ. The psychosocial development of children with cancer is embedded in the research program of prof. dr. M. Grootenhuis, with research programs for anxiety and stress reduction, neuropsychology, communication and sleep in children with cancer. An online monitoring of Health Related Quality of Life is done using the
. By using the KLIK method, problems can be identified and discussed early. In addition, relevant interventions can be offered to teach children how to cope with their disease and to support parents of children with a chronic or life threatening disease. Together with Prof. dr. E. van de Putte, prof. dr. M. Grootenhuis and dr. S. Nijhof the program
has been started. With a non-categorical approach to chronic diseases/cancer during childhood more can be achieved in collaboration. Many studies in pediatric psychology have shown that most important predictors of psychosocial outcomes are not medical factors but the mediating factors such as coping, self-esteem, need for information and social support.
Patient participation uitklapper, klik om te openen
Being a disease with many acute and late effects of tumor and treatment in many different areas of development, research development takes place together with different patient advisory boards. For all children with cancer, representation is given through collaboration with the parent organization VOKK. For supportive care and survivorship research we collaborate with VOKK and VOX; For thyroid carcinoma in children, collaboration has been found with the Stichting Schildklier Onderzoek Nederland. For children with craniopharyngioma and pituitary disease, excellent collaboration is present with the Hypofyse Stichting with a 2-yearly patient representative day. Close collaboration is also running with Stichting Semmy and Villa Joep. Patient representatives play an important role in prioritizing research program, reviewing screening recommendations, and funding application. For children with thyroid cancer and craniopharyngioma, the Cyberpoli has been started through which children can easily ask questions to professionals on the website and have quick access to easily written patient information especially for children.