Group Teske
Group Teske
Cardiomyopathy is a condition of the heart where the heart muscle becomes enlarged, thickened and rigid and patients present with many different symptoms and complaints. As their condition worsens, patients experience electrical problems in their heart leading to irregular heartbeats. We study cardiac mechanics and look at behavior patterns of the heart in order to determine different types of pathological problems underlying heart disease and to develop non-invasive treatments.
More sensitive measuring tools for heart disease
Conventional evaluation of heart function is done by echocardiography, which makes a sonogram (ultrasound) of the heart. This measure volume-based ejection (contractile) function of the heart muscle, and interpretation can vary depending on the person administering it. Recently, more advanced deformation techniques have evolved that are able to track and measure the shortening, lengthening and thickening of heart muscle in particular regions of the heart. My group uses clinical speckle tracking echocardiography (or deformation imaging) on patients with cardiomyopathies.
Cardiomyopathies
Patients with genetic cardiomyopathy display particular heart muscle contraction behavior, which may be able to tell us the prognosis of the disease. One of the strengths of deformation imaging is that we can see, at an early stage, abnormalities in heart muscle function, when on a conventional echocardiogram everything seems normal.
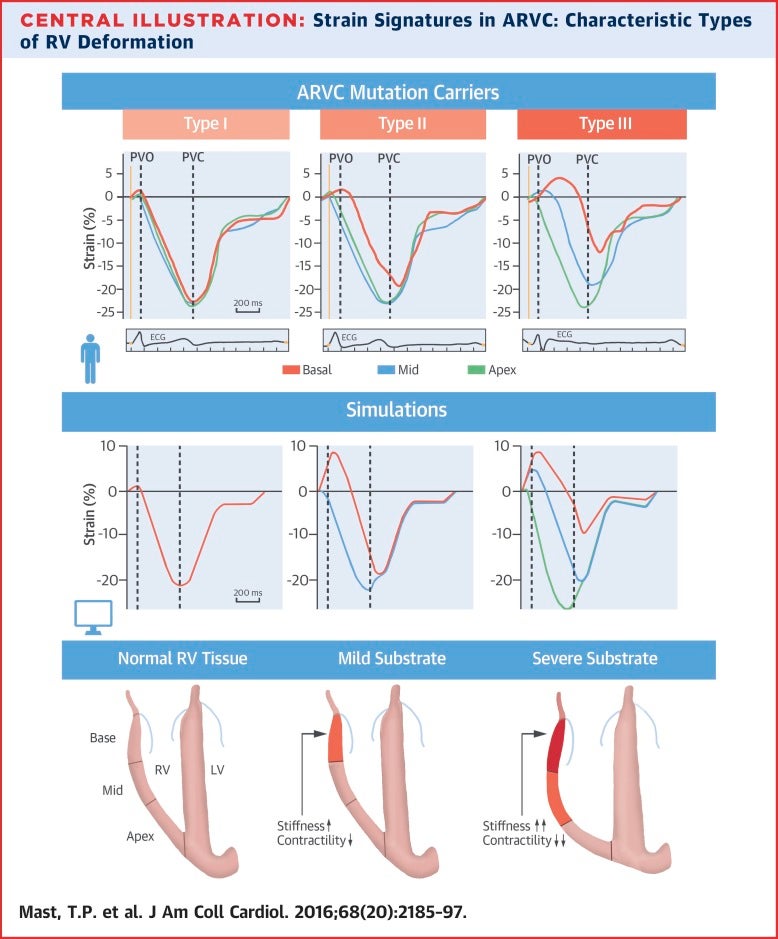
We’re working together with groups in Maastricht and Norway to translate this technique onto a clinical setting, through a computational model that can simulate cardiomechanics when scarring occurs or heart muscle cells are lost. We can make electrical adjustments in the theoretical myocardium to mimic the underlying pathology of patients with cardiomyopathy to analyze the effects of such changes. For example, we’ve seen that we can only simulate arrhythmogenic cardiomyopathy (a rare type of cardiomyopathy) if we induce both fibrosis and kill off heart muscle cells.
In addition, we can use clinical speckle tracking echocardiography to predict those at high risk of developing arrhythmias and heart failure, and perhaps provide evidence for administering interventions or treatment earlier. In a recent publication, we tested several imaging techniques on patients with arrhythmogenic cardiomyopathy. We discovered that echocardiographic deformation imaging could detect electrical and structural abnormalities in these patients, even at early stages, when conventional techniques could not. We’re now validating our results in another patient cohort to look at the prognostic value.
Cardio-oncology
Patients with a healthy heart may receive treatment that damages their heart, such as chemotherapy from which, they develop heart failure. We’re using deformation imaging to identify which patients may be early in the process of developing heart failure as a result of medical treatment and hope to set up an intervention trial for these patients.
We’re also curious as to why some patients get heart failure and others not. We have two comparable patient groups with the same baseline characteristics. However, it’s clear that one group is more prone to cardiac damage after exposure to chemotherapy, and we’re following up on this observation with deformation imaging, biomarkers and genetic analysis.
Research team uitklapper, klik om te openen
Principal Investigator
UMC Utrecht
S. Chamuleau, MD, PhD
M.J. Cramer, MD
B.K. Velthuis, MD, PhD
PhD candidates
J.A Kamphuis, MSc
K. Taha, MSc
F Kirkels, MSc
M. Linschoten, MSc
Maastricht University:
J. Lumens, MD
T. Delhaas, MD, PhD
University of Olso
K Haugaa, MD
T Edvardsen, MD, PhD
PhD candidate
O.H. Lie, MSc

