Musculoskeletal Tissue Regeneration
Musculoskeletal Tissue Regeneration
Within the theme Musculoskeletal Tissue Regeneration, we focus on bone and cartilage tissue engineering, and maxillofacial bone regeneration (the face, mouth, and jaws).
As we age, normal wear and tear of cartilage and/or bone can have an enormous impact on patients, physically, emotionally and financially. Healthy cartilage and bone can be affected by genetics, disease, poor nutrition, infection and trauma. We focus on integrating biology and technology to renew and replace cartilage and bone. The most common joint disease worldwide is osteoarthritis (OA), which occurs when the rubbery cartilage cushion between joints wears down. As OA progresses, patients experience stiffness, swelling, pain and reduced mobility. Eventually, the bones themselves break down, pieces may chip off and float around and in final stages of OA, all cartilage in the joint is gone, and the two boney ends rub directly against each other. Sadly, there is no curative treatment for OA, only pain management or joint replacement. At the other end of the spectrum, is acute injury, for example from a bike accident (broken jaw) or a cartilage tear that occurs when the knee of a soccer player is side-swiped. Young adults have a life-time of movement ahead of them, and in Utrecht, we’ve created a breakthrough therapy in cartilage regeneration, through the IMPACT clinical trial. Survival and proper functioning of implants depend on a network on blood vessels. It’s important to realize that cartilage does not have its own vasculature (blood supply); the subchondral bone (bony parts just under the cartilage) provides this in order to maintain the health of our joints. Without a blood vessel system, regeneration potential is severely reduced. In Utrecht, we study a range of methods to improve pain management, to kick-start our natural regeneration potential, to design better bone and cartilage implants, to generate new blood vessels and to create 3D environments for making new tissue.
For a better view of our work have a look on a few examples following below.
Making bone uitklapper, klik om te openen
The long bones of our bodies (think of your arms and legs) support most of our weight and help us move. They’re formed when bone cells and blood supply invade cartilage and lay down mineral deposits. We’re mimicking the natural developmental process of these bones by implanting cartilage cells and letting our body transform them into bone. What’s unique about our approach is that we’re testing this system with unmatched immune systems. This means that we could use cartilage cells from a donor. Another method we’re exploring is the use of dental pulp stem cells, which are found in the middle of each tooth. We’re trying to determine if these cells can contribute to the regenerative process of bone. Both methods, if successful, would mean that patients would not need a painful bone aspiration procedure prior to replacement surgery.

Chronic back pain and regeneration uitklapper, klik om te openen
Intervertebral discs (IVD) act as shock absorbers for our spine. Anyone with chronic back pain can attest to their importance. We’re studying notochordal cells, a special type of cell present in the IVDs of children up until 10 years of age; after that, they’re replaced by chondrocyte-like cells. We’re trying to mimic natural developmental processes and hope that these cells can boost IVD regeneration. In addition, we’re combining this hypothesis with a more recent discovery that extracellular vesicles (EV) may also enhance regeneration. EVs are small, membrane-enclosed particles released by cells that play a role in cell-to-cell communication. As their name suggests, they can potentially be great carriers of potent factors that can stimulate IVD regeneration.
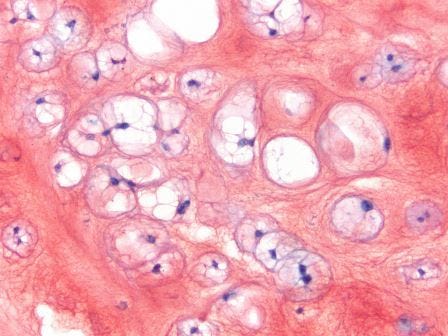
Osteoarthritis: better pain management and regeneration uitklapper, klik om te openen

It’s ironic that it’s often painful to receive pain medication. We’re developing a drug delivery-based treatment, consisting of biodegradable microspheres and FDA-approved drugs, that can steadily deliver pain medication over a long period of time, inside the diseased joint, negating the need for multiple doctor’s visits and injections. Using a knee osteoarthritis (OA) model and a model of intervertebral disc degeneration, we hope to create a system that delivers pain medication specifically to the synovial lining of the knee and to the painful IVD without systemic aside effects. It’s exciting to see that we can reduce both pain and stimulate regeneration in our preliminary in vivo studies in rats and canines. We’ve observed this in both OA and intervertebral disc degeneration by a decrease in inflammation and an increase in healthy tissue. Our next steps are to conduct a clinical trial on lower back pain and OA in canine patients with naturally occurring degenerative joint disease.
3D printing and biofabrication uitklapper, klik om te openen
Biofabrication is the convergence of medicine, biology, chemistry and engineering. Our ultimate goal is to create living tissues in the lab, through automated fabrication processes and 3D cell culture. In Utrecht, we combine materials with cells to create an excellent environment for cells to live in. We aim to produce tissues as replacements for damaged tissues, or as models for drug efficacy. The key to this is to combine materials and stem cells in a 3D architecture as similar as possible to the that of native organs. The Utrecht Biofabrication Facility pushes the boundaries of this new field. One example is our 3D-Joint project, which focuses on the knee. We’ve designed a new approach, and we’re the first to combine both cartilage and bone regeneration simultaneously, using biofabrication methods that permit the printing of cells together with micrometer and nanometer-sized fibers, closely mimicking the matrix in bone and cartilage. What’s exciting is exploring the unknown and testing our ideas. We have a wide range of advanced fabrication techniques in Utrecht, and the unique ability to make virtually any shape with any combination of cells and materials.

A 3D bone marrow niche uitklapper, klik om te openen
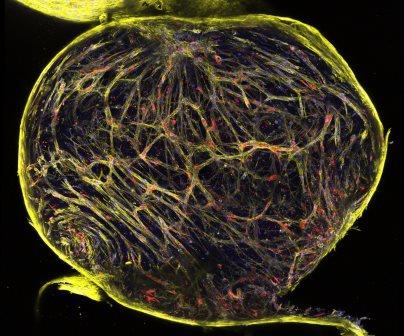
Multiple myeloma cancer patients end up in the orthopaedics department because of bone lesions and pathological fractures. While chemotherapy can be effective against this disease, a debilitating side effect is that the cancer cells change MSCs such that they can no longer regenerate. Multiple myeloma cells are dependent on the surrounding bone and bone marrow for their survival, and cannot be cultured on their own. We’ve designed an in vitro 3D model for bone and bone marrow that can sustain these cells twice as long as published models. Using this model, cell interactions can be studied, and therapies can be tested. What’s truly rewarding is that our model enabled the approval of a clinical trial with a new immunotherapy using engineered T-cells to combat multiple myeloma. We’re also exploring this model to sustain and expand HSCs (blood stem cells), and to also study the non-cancerous environment, looking at the influences of different cell types within the bone marrow niche.
The art of air brushing uitklapper, klik om te openen

When you think of airbrushing, you probably think of graffiti artists. We do too, yet we also see this technique as a new, less invasive manner for reconstructive knee surgery. If you undergo surgery, it means opening up your entire knee. With an airbrush, a surgeon only needs two tiny holes in your knee, one for a camera and one for the airbrush instrument. Using the airbrush, the surgeon can then spray and line the defective area with the appropriate cells and biomaterials. We’ve now built a prototype that takes into account parameters such as cell/biomaterial dimensions, delivery force and instrument weight and size, and will conduct prototype trials to assess the feasibility of this new method of reconstructive surgery.

