May 10: Immunotherapy for high-risk neuroblastoma affects fighting capacity of the immune system

In children with high-risk neuroblastoma, immunotherapy results in both stimulatory and inhibitory effects on the immune system. This finding by researchers from UMC Utrecht and the Princess Máxima Center for Pediatric Oncology in Utrecht provides new insights for improvement of therapy timing as well as new therapy strategies enhancing immune cell fighting capacity.
Neuroblastoma is a type of childhood cancer with a significant risk of mortality. Despite intensive treatment - including immunotherapy - prognosis of high-risk neuroblastoma is still poor. Increasing amounts of research have shown that the fighting capacity of the immune system is important for the outcome of neuroblastoma treatment. However, the patient’s immune status and the effects of immunotherapy on the immune system are often not taken into account. Therefore, researchers at the Center for Translational Immunology at UMC Utrecht in collaboration with the Princess Maxima Center for Pediatric Oncology in Utrecht investigated in detail the fighting capacity of immune cells in the blood of high-risk neuroblastoma patients.
Fighting capacity
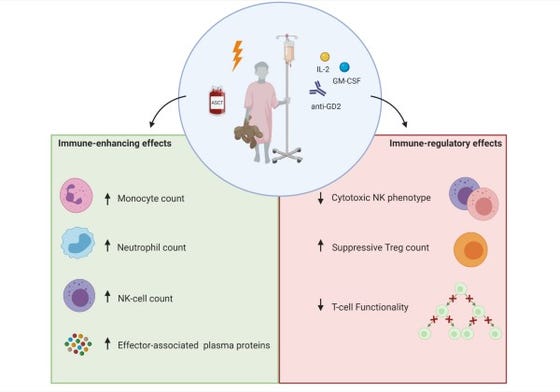
In this study in 25 neuroblastoma patients (median age at diagnosis 3.9 years), the researchers observed both processes that stimulate and processes that decrease the fighting capacity of the various immune cell types including leukocytes, lymphocytes, monocytes, neutrophils, eosinophils and specific lymphocyte subsets (B-cells, NK-cells, T-cells) at diagnosis and during immunotherapy with dinutuximab, a monoclonal antibody targeting the glycolipid GD2 on the surface of neuroblastoma cancer cells. They showed that the overall fighting capacity of the immune system of neuroblastoma patients was impaired at diagnosis as well as during therapy. In addition, the researchers observed considerable interindividual variation, which might explain differences in therapy efficacy between patients.
Translational immunologist and senior author of the publication dr. Stefan Nierkens concluded: “Our study using functional immune monitoring provides insights for improvement of timing of immunotherapy as well as for new therapy strategies that may enhance the immune cell fighting capacity to prevent relapse in children with high-risk neuroblastoma.”
Neuroblastoma
Neuroblastoma is a type of cancer that forms in nerve tissue. Symptoms may include bone pain, a lump in the abdomen, neck, or chest, or a painless bluish lump under the skin. The cancer is divided into risk groups based on age, tumor stage and presence of certain genetic components. Treatment consists of chemotherapy, stem cell transplantation, surgery, local radiation and/or maintenance immunotherapy. Low-risk disease in babies typically has a good outcome with surgery or simply observation. In high-risk disease, the 5-year event-free survival is less than 50 percent, despite aggressive treatment. neuroblastoma is the most common extracranial solid tumor in children, accounting for approximately 15 percent of all pediatric oncology deaths.
Reference
Szanto CL, Cornel AM, Tamminga SM, Delemarre EM, de Koning CCH, van den Beemt DAMH, Dunnebach E, Tas ML, Dierselhuis MP, Tytgat LGAM, van Noesel MM, Kraal KCJM, Boelens J-J, Huitema ADR, Nierkens S. Immune monitoring during therapy reveals activitory regulatory immune responses in high-risk neuroblastoma. Cancers 2021;13:2096
